Boy, was I blindsided?
 I posted a quote from a study that examined the general public’s understanding of hospice on my Hard Choices for Loving People Facebook page. 30% of the respondents said they felt hospice hastens death. My Facebook post got hundreds of likes and comments, a lot of traffic for my humble page. I had no idea this would engender such a strong response.
I posted a quote from a study that examined the general public’s understanding of hospice on my Hard Choices for Loving People Facebook page. 30% of the respondents said they felt hospice hastens death. My Facebook post got hundreds of likes and comments, a lot of traffic for my humble page. I had no idea this would engender such a strong response.
“This morphine is wonderful”
Misconceptions can be based on misconceptions. When people hear that a friend is receiving morphine, they automatically think death is near. Not necessarily. Because of this close association of morphine with death and the association of getting on morphine in hospice, many assume that’s what hospice does — hastens death. Not so. Morphine controls pain and relaxes breathing.
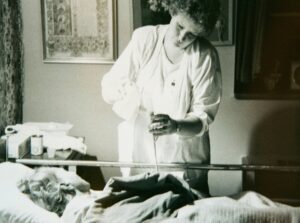
I had an elderly patient once who was dying of respiratory failure. She was so short of breath that it was a major chore for her to move from her bed to a chair. She got great relief from morphine which she took for months before dying. She told me once, “I’ve always been opposed to drugs, but this morphine is wonderful.”
The coincidence of death after morphine
Many of the respondents to my post who agreed that “hospice hastens death” told stories of family members going on hospice and dying soon after. Why should this surprise us? Hospice requires that a patient is within six months of dying, although the average patient is only on hospice for two weeks.
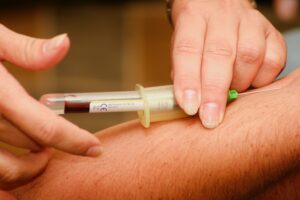
I am sure it is just a coincidence that a patient receives a dose of morphine and dies shortly after. The family then thinks, “she died because they gave her morphine.” She did not. She was on hospice because she was dying, and she just happened to take her last breath after taking morphine.
No incentive for a hospice to hasten death
 It makes no sense that hospice would want to hasten a patient’s death. The more days the patient is on hospice, the more reimbursement the hospice receives. It is totally against their financial interest to hasten death.
It makes no sense that hospice would want to hasten a patient’s death. The more days the patient is on hospice, the more reimbursement the hospice receives. It is totally against their financial interest to hasten death.
Hospices also want to make sure their patients are as pain-free as possible. Families of hospice patients fill out surveys after the death of their person. They rate the hospice on pain control, among other items.
So, yes, hospices use morphine to keep patients comfortable, not hasten death. They want to have the patient as long as a natural dying process will allow, and they want favorable survey results.
The research is clear; patients live longer on hospice
 Many studies confirm that hospice patients live longer than nonhospice patients suffering from the same disease. One study looked at dementia patients. On average, the patients on hospice lived longer than those who never entered a hospice program.
Many studies confirm that hospice patients live longer than nonhospice patients suffering from the same disease. One study looked at dementia patients. On average, the patients on hospice lived longer than those who never entered a hospice program.
Another study looked at five different kinds of cancer and congestive heart failure. Once again, the patients who were under hospice care lived longer than the nonhospice patients.
So, rest easy. If you have a life-limiting illness and want to live longer with a better quality of life, go into hospice as soon as possible.
________________________________________
Chaplain Hank Dunn is the author of Hard Choices for Loving People: CPR, Feeding Tubes, Palliative Care, Comfort Measures and the Patient with a Serious Illness and Light in the Shadows. Together they have sold over 4 million copies. You can purchase his books at hankdunn.com or on Amazon.



 Recently,
Recently,  Then, of course, “happy” is
Then, of course, “happy” is  Recently, I
Recently, I 

 “Charlie” was not a very creative name, but it just seemed to fit a male King Charles Spaniel. At first, we crated him at night. After weeks of barking, he finally settled into his crate and his place at home. Until…
“Charlie” was not a very creative name, but it just seemed to fit a male King Charles Spaniel. At first, we crated him at night. After weeks of barking, he finally settled into his crate and his place at home. Until… Charlie joined Katie in Oxford her second year at Ole Miss, where he supported her during roommate issues and dating cycles. Their deep bond reached new depths. A dog just loves unconditionally.
Charlie joined Katie in Oxford her second year at Ole Miss, where he supported her during roommate issues and dating cycles. Their deep bond reached new depths. A dog just loves unconditionally.

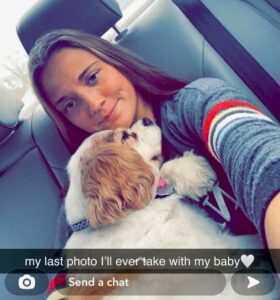 On Sunday afternoon, my wife and I were pulling into the Walmart parking lot, and she blurted out, “Katie has to come home tonight.” It was a mother’s flash of insight for her soon-to-be grieving daughter. She called Katie and told her to get to National airport and get on a plane. I picked her up in Memphis with Charlie a few hours later. They slept together on our bedroom floor that night before she returned to D.C., Monday. In the car on the way to the Memphis airport, she “Snapped” a photo to friends, “my last photo I’ll ever take with my baby.” Indeed, it was.
On Sunday afternoon, my wife and I were pulling into the Walmart parking lot, and she blurted out, “Katie has to come home tonight.” It was a mother’s flash of insight for her soon-to-be grieving daughter. She called Katie and told her to get to National airport and get on a plane. I picked her up in Memphis with Charlie a few hours later. They slept together on our bedroom floor that night before she returned to D.C., Monday. In the car on the way to the Memphis airport, she “Snapped” a photo to friends, “my last photo I’ll ever take with my baby.” Indeed, it was.


 About that same time, I started traveling around the country making presentations to healthcare professionals. My most popular talk, “Helping Patients and Families with End-of-Life Decisions,” includes a series of slides with “Hank’s Theorems” on various end-of-life issues. The first slide says, “The peacefulness of a death is directly proportional to the distance from the hospital ICU.”
About that same time, I started traveling around the country making presentations to healthcare professionals. My most popular talk, “Helping Patients and Families with End-of-Life Decisions,” includes a series of slides with “Hank’s Theorems” on various end-of-life issues. The first slide says, “The peacefulness of a death is directly proportional to the distance from the hospital ICU.”

 The Journal of the American Medical Association recently published an opinion piece,
The Journal of the American Medical Association recently published an opinion piece, 




