275K followers on YouTube, 432K on Instagram, and 919K on TikTok. With numbers like these, @hospicenursepenny is an INFLUENCER.
 Penny Hawkins Smith, RN, educates and entertains (yes, entertains) her followers with short videos (okay, “reels”) based on her experience as a hospice nurse. She now has brought her earthy take on death, dying, and hospice to written form in her book, Influencing Death: Reframing Dying for Better Living.
Penny Hawkins Smith, RN, educates and entertains (yes, entertains) her followers with short videos (okay, “reels”) based on her experience as a hospice nurse. She now has brought her earthy take on death, dying, and hospice to written form in her book, Influencing Death: Reframing Dying for Better Living.
Spare me a moment of shameful self-promotion — my Hard Choices for Loving People is one of just four books she recommends in her “Resources” section…I digress.
Like many of us in hospice work, Nurse Penny has learned how to live a better life as she watched her patients and their families navigate the journey unto death. In her words, “Being present with the dying and those they love has brought me joy, happiness, meaning, and purpose.”
HelpMeLeaveMyHusband.com
 This outlook did not come easy for her. This book is, in part, a memoir about how a troubled young mother survived her own addictions and reckless living. Her life story is woven into the fabric of a book to help people have a better death and, she hopes, have a better life.
This outlook did not come easy for her. This book is, in part, a memoir about how a troubled young mother survived her own addictions and reckless living. Her life story is woven into the fabric of a book to help people have a better death and, she hopes, have a better life.
It turns out that Smith was an internet sensation long before TikTok and Instagram. With her first marriage dissolving and having child-rearing and nursing school expenses, she set up a website (no longer active), HelpMeLeaveMyHusband.com. This led to national publicity, including an interview on “The View” and a mention in Time magazine. Who knew?
Practical advice on having a “good death”
The real power in this book comes from the stories of her patients, their families, and her own journey with death in her family. Because of her large platform, Nurse Penny has a good read on what people currently think about death, fear of it, and how to prepare for it.
 Questions and comments from Smith’s social media followers appear in Influencing Death, allowing segues to practical end-of-life advice. Here are just a few nuggets of Penny’s wisdom found in these pages:
Questions and comments from Smith’s social media followers appear in Influencing Death, allowing segues to practical end-of-life advice. Here are just a few nuggets of Penny’s wisdom found in these pages:
- “The earliest signs [that death is near] are eating less, sleeping more, and socially withdrawing.”
- “[T]he reality is that thinking about our inevitable demise, accepting it, and planning for it are the best ways to have a good death.”
- “People seem to think that saying words like ‘death,’ ‘dying,’ ‘died,’ or ‘dead’ will cause it to happen. Death is what it is, and calling it by another name won’t change that outcome.”
- “No, they don’t need to eat. They’re dying, and they aren’t dying because they’re not eating. They’re not eating because they’re dying!”
- “He, like many, many family members of hospice patients, was worried that he would cause her to die faster by giving her morphine. I’ll reiterate for the people in the back that this couldn’t be further from the truth.”
- “Being present with the dying and those they love has brought me forgiveness—forgiveness for the people who hurt me and, more importantly, forgiveness for myself.”
“Is there an afterlife?”
When I started work as a hospice chaplain in 1996, two nurses at our agency had authored what became a very popular book, Final Gifts. Maggie Callanan and Patricia Kelley told stories of patients having deathbed visions or telling family members they were going to “take a trip.” It is still selling 33 years later.

Photo by Aamir Suhail on Unsplash
Fast forward to now, when Penny Smith (and two other social-media-influencer-hospice-nurses-turned-authors) address these fascinating phenomena and delve into the question, “Is there an afterlife?” Smith recounts many of these stories in a chapter titled “The Woo-Woo Stuff.”
All these influencer-nurse-authors tell similar stories of dying patients having visions or dreams of dead relatives coming to visit them. These visions are very comforting to patients, although sometimes discomforting to their families. Nurse Penny adds her own experience… read the book to find out how that goes.
Penny is very clear that she does not believe in God, nor does she practice religion. At the same time, she is also clear that observing these deathbed visions and having had her own experience, she believes that we do still exist after death.
Are these visions “real?” That’s not even a good question. They are “real” to the people who experience them. That should be the bottom line.
Thank you, Sergeant
Penny’s story takes us through some very dark places of her addiction journey, including when she spent a night in jail. The next morning, the police sergeant told her, “You are not the same person who came in here last night. You seem very bright. Why are you here? I really hope you can get on the right track because it seems like it would be such a waste if you didn’t.”
I was touched to see him listed with others in the “Acknowledgments” at the end of the book: “The sergeant at the police station, I’m sure I will never see you again, but I do hope if by chance you read this book, you will know how ultimately life-changing your words were.”
I, too, thank the sergeant.
__________________
Author Chaplain Hank Dunn, MDiv, has sold over 4 million copies of his books Hard Choices for Loving People and Light in the Shadows (also available on Amazon).
Follow Hank: LinkedIn | Instagram | Facebook | YouTube



 My wife and I were signing papers in the VW sales office when we noticed a long line of people holding propane tanks across the street. My wife commented, “Look at all the people getting ready to grill on Labor Day.” The salesman responded, “Are you crazy? They’re getting ready for the hurricane.”
My wife and I were signing papers in the VW sales office when we noticed a long line of people holding propane tanks across the street. My wife commented, “Look at all the people getting ready to grill on Labor Day.” The salesman responded, “Are you crazy? They’re getting ready for the hurricane.”


 “When I’m dead, I’m dead.… and I just sail off into nothingness, and that brings me a lot of comfort. That doesn’t bring everyone comfort but it brings me comfort.” —Caitlin Doughty, author of
“When I’m dead, I’m dead.… and I just sail off into nothingness, and that brings me a lot of comfort. That doesn’t bring everyone comfort but it brings me comfort.” —Caitlin Doughty, author of 



 I have just discovered two great videos with Dr. Michael Greger discussing this very topic. Each video is less than seven minutes and worth every minute of your time. One is called
I have just discovered two great videos with Dr. Michael Greger discussing this very topic. Each video is less than seven minutes and worth every minute of your time. One is called 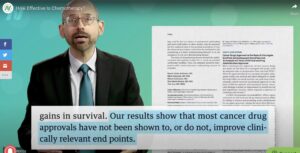 In his second video he referred to a study reported in the Journal of the National Cancer Institute. “In fact, the most expensive drug they looked at, the one costing $169,836 a year, did not improve overall survival at all, and actually worsened quality of life. That’s $169,000 just to make you feel worse with no benefit. Why pay a penny for a treatment that doesn’t actually help?”
In his second video he referred to a study reported in the Journal of the National Cancer Institute. “In fact, the most expensive drug they looked at, the one costing $169,836 a year, did not improve overall survival at all, and actually worsened quality of life. That’s $169,000 just to make you feel worse with no benefit. Why pay a penny for a treatment that doesn’t actually help?” Searching for Stars on an Island in Maine
Searching for Stars on an Island in Maine Almost Human: The Astonishing Tale of Homo Naledi and the Discovery That Changed Our Human Story
Almost Human: The Astonishing Tale of Homo Naledi and the Discovery That Changed Our Human Story The Home Place: Memoirs of a Colored Man’s Love Affair with Nature
The Home Place: Memoirs of a Colored Man’s Love Affair with Nature Useful Delusions: The Power and Paradox of the Self-Deceiving Brain
Useful Delusions: The Power and Paradox of the Self-Deceiving Brain Illness as Metaphor (1978) and AIDS and Its Metaphors (1989
Illness as Metaphor (1978) and AIDS and Its Metaphors (1989
 A
A 
 The Journal of the American Medical Association recently published an opinion piece,
The Journal of the American Medical Association recently published an opinion piece, 
 Rev. Lynn Casteel Harper of the Riverside Church in New York City, sees her role with congregants in their decline as one of “presence and witness.” “Sometimes if people are going through really difficult experiences, especially medically, it’s easy for the story of the illness and the suffering to take over,” Rev. Harper said. “Part of my role is to affirm the other dimensions.”
Rev. Lynn Casteel Harper of the Riverside Church in New York City, sees her role with congregants in their decline as one of “presence and witness.” “Sometimes if people are going through really difficult experiences, especially medically, it’s easy for the story of the illness and the suffering to take over,” Rev. Harper said. “Part of my role is to affirm the other dimensions.”